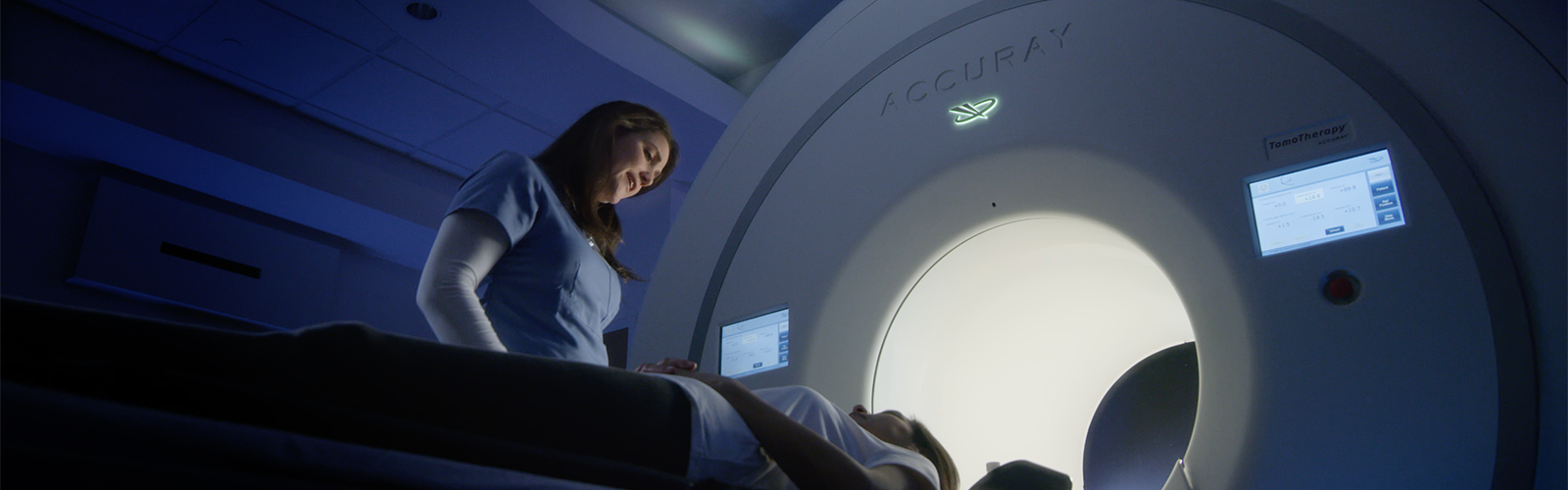
Welcome to the Department of Human Oncology (DHO) at the University of Wisconsin
We provide comprehensive radiation oncology services with dedication to improve the outcome for cancer patients using state-of-the-art treatment techniques combined with highly compassionate care. Our clinical focus is on each individual cancer patient and their families; however, our mission extends more broadly to include cutting-edge research and advanced training for the next generation of MD and PhD students to ensure cancer therapy improvements for the future.
Paul M. Harari, MD, FASTRO
Jack Fowler Professor and Chairman
Department of Human Oncology
NEWS
 ACRO announces DHO’s Jessica Schuster, MD as URiE Editor-in-Chief
ACRO announces DHO’s Jessica Schuster, MD as URiE Editor-in-Chief
The American College of Radiation Oncology is proud to announce the leadership for CURiE: Contemporary Updates: Radiotherapy Innovation & Evidence, a cutting-edge publication through the Cureus Journal of Medical Science.
Jessica Schuster, MD, FACRO will serve as CURiE Editor-in-Chief.
 Faculty, Residents and APPs 2023
Faculty, Residents and APPs 2023
A framed version of this 2023 DHO formal photograph (and multiple prior years) was mounted this week in the Radiation Oncology clinic and K4/4th floor DHO administrative hub. Take a brief tour of these images anytime.
 Dr. Bhudatt Paliwal marks 50 years of cancer research excellence
Dr. Bhudatt Paliwal marks 50 years of cancer research excellence
In the world of medicine, some individuals stand out not only for their knowledge and expertise but also for their unwavering commitment to innovation and improving the lives of patients. Dr. Bhudatt Paliwal, professor emeritus in the Departments of Human Oncology and Medical Physics, is one such luminary: he is celebrating 50 years of helping to advance life-saving discoveries in cancer research and radiation therapy.
 Dr. Anderson presents at NRG Oncology conference
Dr. Anderson presents at NRG Oncology conference
At the July NRG Oncology conference in Philadelphia, Dr. Anderson provided a “Radiation 101” presentation to over 400 NRG Oncology Clinical Research Associates and Clinical Research Nurses.
 DHO Graduating Residents’ Farewell 2023
DHO Graduating Residents’ Farewell 2023
The Department of Human Oncology recently celebrated three incredibly talented resident graduates at Cooper’s Tavern to honor completion of their training programs in June 2023. Christina Breeze, Emily Merfeld and Lindsay Bodart were lavished with praise and certificates commemorating their milestone achievements.

Dr. Quaovi Sodji completes his Bentson Fellowship
Dr. Quaovi Sodji recently completed his Bentson Translational Research Fellowship at the University of Wisconsin in the Department of Human Oncology. Dr. Sodji has now been recruited to join the faculty of the Department of Human Oncology as a tenure-track assistant professor and he will continue his translational research here.
 Dr. Ben Durkee wins Educator of the Year Award
Dr. Ben Durkee wins Educator of the Year Award
Dr. Benjamin Durkee recently received the 2022 – 2023 Association of Residents in Radiation Oncology (ARRO) Educator of the Year Award. This distinguished recognition celebrates Dr. Durkee’s dedication to teaching and mentoring residents.
 Four DHO Undergraduate Researchers Win Awards in Summer 2023
Four DHO Undergraduate Researchers Win Awards in Summer 2023
The Department of Human Oncology (DHO) is dedicated to mentoring undergraduate researchers. By working in the department’s labs, students learn from world-class scientists, contribute to the department’s research agenda, and gain experience that can have a lasting impact on their future careers. This year, four undergraduates who work with DHO scientists have recently been recognized for their research.
 Dr. Peter Mahler Retires after 32 years as a Cancer Physician/Scientist
Dr. Peter Mahler Retires after 32 years as a Cancer Physician/Scientist
Professor Peter Mahler, PhD, MD, Department of Human Oncology, retired on February 28, 2023 after a long association with the University of Wisconsin. His career has taken him from the Midwest to the Eastern Great Lakes to the West Coast and then back to Wisconsin.
Find Us in the Community
Wisconsin Head and Neck Cancer SPORE
The Wisconsin Head and Neck SPORE is designed to promote translational laboratory and clinical research to improve overall outcome for patients with Head and Neck Cancer (HNC).
Badger Challenge for Cancer Research: September 24, 2023
Thank you to all riders and supporters for Badger Challenge 2022! We had another record year, bringing us to nearly $2.6 million!
2022 Milestones:
$802,761 raised for cancer research
2,751 registered riders
350 volunteers