The following are descriptions of several adaptive radiotherapy research projects that our medical physicists are currently pursuing:
MRI-guided Adaptive Radiation Therapy
MRI-guided radiation therapy provides a method by which we are able to observe daily changes in the patient’s internal anatomy. This can be caused by many factors, ranging from reduction in tumor size to differing amounts of content in the stomach, bladder and bowels. Consequently, radiation treatment plans based on an image acquired weeks prior to radiation delivery may not adequately represent the patient’s anatomy on a daily basis.
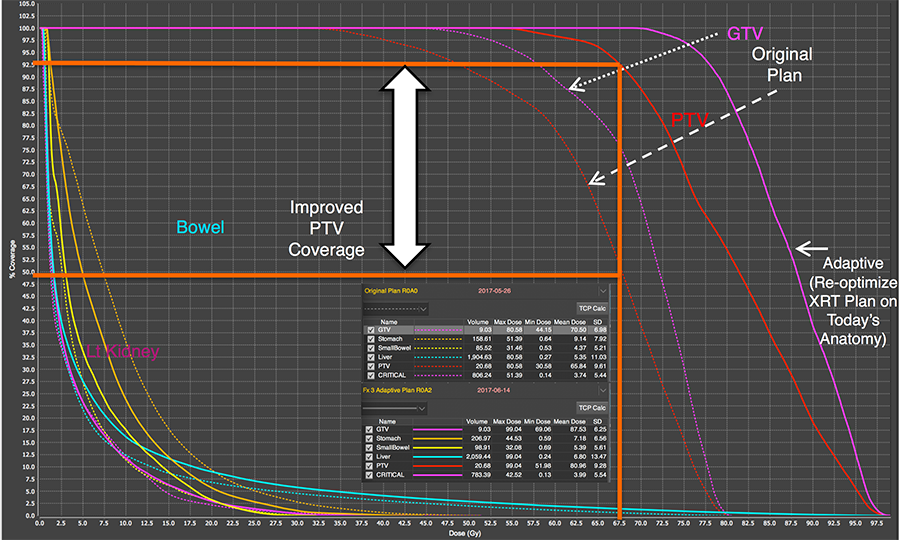
MRI-guided Adaptive Radiation Therapy is a process through which we can identify these anatomical changes and adapt the patient’s treatment on a daily basis, which can produce a substantial improvement in the radiation dose distribution. The image below shows a Dose Volume Histogram for two treatment plans, the original plan and an adaptive plan. The adaptive plan shows much better radiation dose delivery to the gross tumor volume (GTV) and planning tumor volume (PTV) when compared to the original plan. The doses to normal tissues are also reduced with the adaptive plan. We are investigating novel planning techniques to make this process robust and effective.
Commissioning and Implementation of MR-Guided Online Adaptive Radiotherapy (ViewRay MRIDIAN System)
Adaptive radiotherapy (ART) addresses the variability of patient anatomy, either random or systematic interfraction changes. Online ART allows the ability to dynamically change the treatment plan during a treatment session. Dose-guided radiotherapy through online ART permits dose escalation/de-escalation when dose limiting organs at risk have moved away/closer to the target. The paradigm of online, on-table adaptive radiotherapy is now clinically achievable with MR-guided radiotherapy.
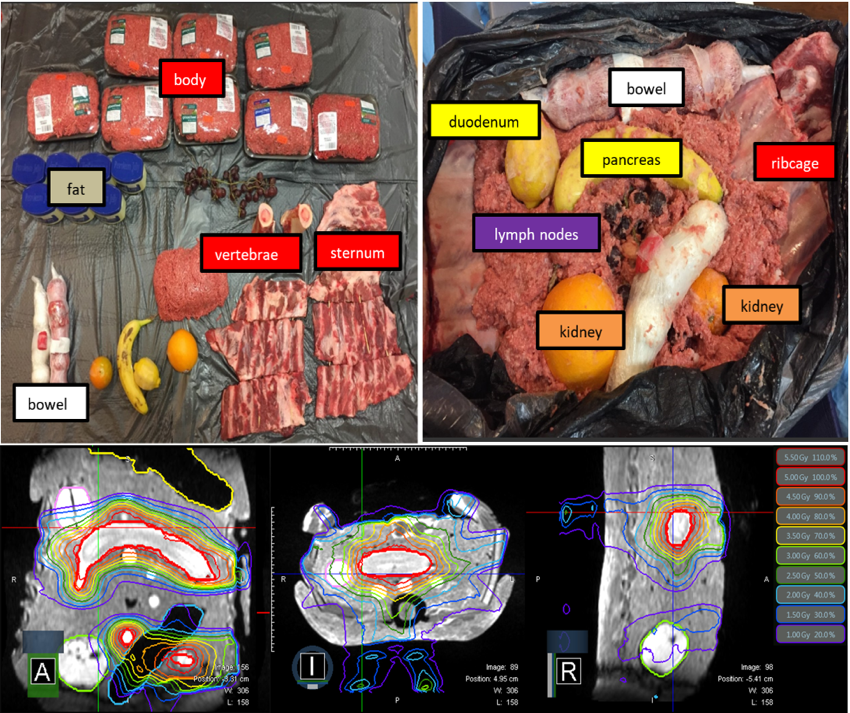
In 2017 we implemented MR-guided online adaptive radiotherapy at the University of Wisconsin on the MRIdian (ViewRay, Inc., Cleveland, OH). Prior to clinical release, our physics team validated the safety and accuracy of the ART program. Our commissioning process included validation of the deformation and the dosimetric accuracy with an in-house heterogeneous phantom (Figure). We reported our findings of the online adaptive dosimetric and deformable accuracy and the validation of online adaptive workflow processes at the 2017 AAPM Annual Meeting.
Indications for Online Adaptive Radiotherapy Based On Dosimetric Consequences of Interfractional Pancreas-To-Duodenum Motion in MRI-Guided Pancreatic Radiotherapy
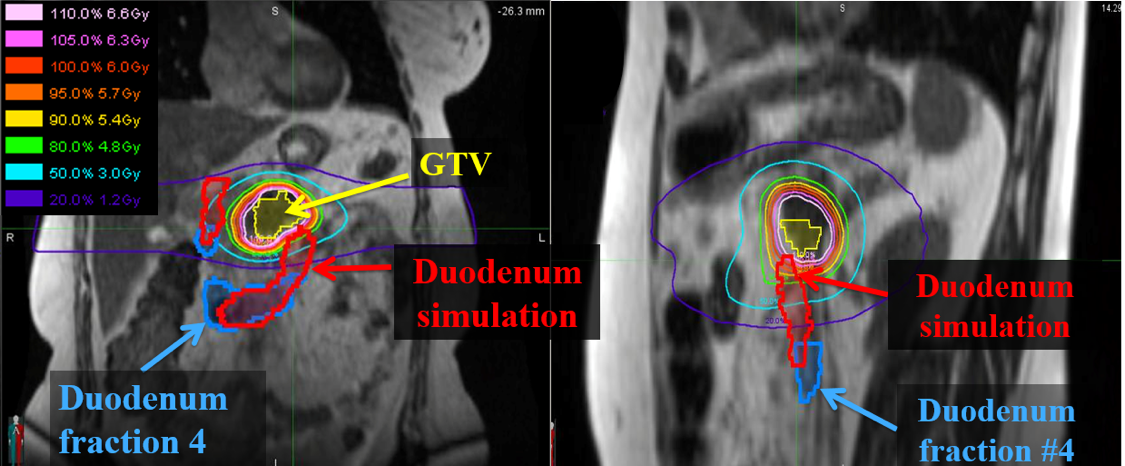
Dose-limiting structures, such as the duodenum, render the treatment of pancreatic cancer challenging. In this multi-institutional study, we assess dosimetric differences caused by interfraction pancreas-to-duodenum motion using MR-IGRT to determine the potential impact of adaptive replanning.
In this work, we evaluated the indication for adaptation through evaluation of pancreas-to-duodenum interfraction motion. Adaptation was considered indicated when daily positional variations enabled dose escalation to the target while maintaining duodenal constraints. Dose escalation through online adaptation was found feasible in MR-guided pancreatic radiotherapy for fractions where GTV-to-duodenum distance increased from simulation. We reported our findings at the 2016 AAPM and ASTROAnnual Meeting.
IMPLICATIONS FOR ONLINE ADAPTIVE AND NON-ADAPTIVE RADIOTHERAPY OF GASTIC AND GASTROESOPHAGEAL JUNCTION CANCERS USING MRI-GUIDED RADIOTHERAPY
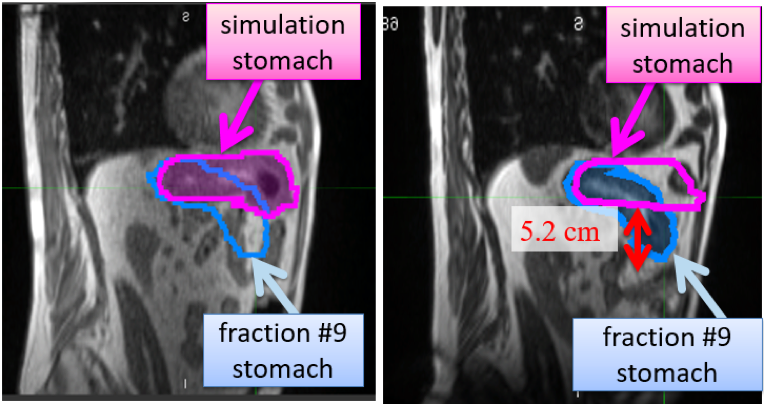
Stomach anatomy is susceptible to large interfraction motion and deformation (Figure). Thus, large treatment margins have historically been used for the treatment of gastric and gastroesophageal junction (GEJ) tumors at the expense of heathy, normal tissues. In this work we evaluated the role of adaptation as well as the margin determination in non-adpative radiotherapy.
To this end, we quantified the interfraction motion and deformation in gastric and GEJ patients undergoing MR-guided radiotherapy. We observed notable interfractional change in daily stomach shape in both gastric and GEJ patients, for which adaptive radiotherapy is indicated. Details of our findings were reported at the 2016 AAPM Annual Meeting.